Through radical transparency and community rewards, HealthTap aspires to become the default national rating and search destination for patients seeking physicians. If it can better match patients to treatments and doctors than Google, then it's well on its way.

Though the Internet has opened up access to much of world's information, finding a specialist for medical advice still requires the age-old process of personally asking a doctor to suggest a trusted colleague. "There's just no way in the world to do it right now, short of going to a primary care physician," says HealthTap founder Ron Gutman, who wants to expose the hidden knowledge that exists among practicing doctors about who the best physicians are for specific treatments.
HealthTap, a medical social network for users seeking personalized, public advice from registered doctors, tells Fast Company that it is releasing an eBay-like rating system for its more than 10,000 participating doctors and their relevant expertise. We spoke with Gutman about how his system has incentivized doctors to go against the taboo of cricitizing their peers, how transparency brings credibility to online medical advice, and how HealthTap translates conversational descriptions of symptoms into medical language their doctors can respond to.
Incentivize Against Taboos
"Physicians are very loath to criticize each other, for fear that they will be criticized themselves," says Dr. Geoff Rutledge, HealthTap's Chief Medical Information Officer, who was a Harvard medical researcher before being executive at Healtheon, which eventually became WebMD. The taboo against public naysaying, argues Rutledge, has kept the Internet at bay, while other industries are transformed by more openness.
HealthTap's solution to encourage doctors to evalute their colleagues was to keep everything positive: Doctors can either agree with a solution proposed by a colleague or offer their own. As with Facebook, on HealthTap, there is no "dislike" button. "By defining everything that's good, you can then choose among all the best answers, without having this aura or fear that individuals are being criticized."
Racking up kudos like gold coins in Mario Brothers feeds the ever-present desire for repute in the medical community and a steady supply of patients. As HealthTap grows in size, and reels in more prestigious doctors (Harvard Medical School is the most popular school in the network), HealthTap has the aim of being the most comprehensive national ranking system for doctors.
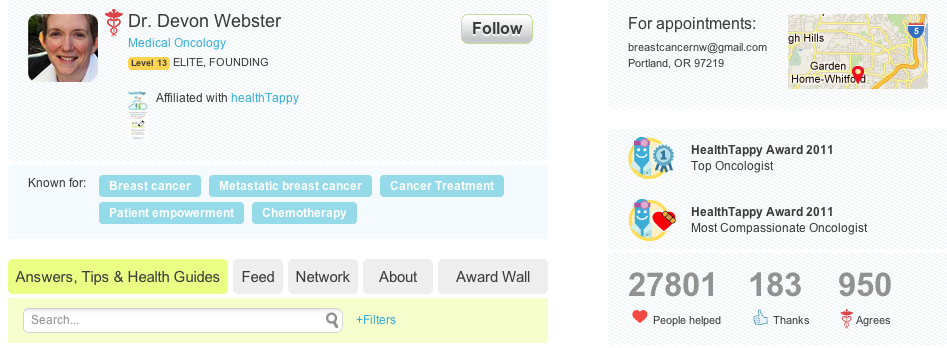
The user interface itself is decked out in referral buttons and awards galore. Answers are accompanied by a giant "thank" button in the top right hand corner, and a doctor's avatar is decorated like a military uniform, with their HealhTap score and expertise placed directly under their name. The doctor profile pages themselves prominently display the total number of patients they've reached, how many lifetime "thanks" and "agrees" they received. Like a wall of plaques in their office, the profile page prominently displays HealthTap's own version of awards, some as silly as the "Healthcliff Huxtable award" for receiving 50 total "thanks."
The new "Docscore" will tally all of this into a number, and include "a physician’s network (i.e. what other physicians the doctor in question follows and vice versa, as well as the number and nature of interactions within the network). The number of physicians who refer patients or content to a particular doctor is also taken into account, along with a variety of trust-related data points collected about the physician from other online resources," according to Gutman.
In other words, HealthTap aspires to create the national rating sytem for doctors and their expertise, using their own proprietary measures, making them the default rating for medical advice.
Yet, the cacophony of awards and ratings begs the question of whether HealthTap's ratings reflect a doctor's actual quality.
Community Truth
"At the end of the day, what you are getting as a patient is the physician's community opinion on a certain question," says Gutman. HealthTap, he says, can't objectively verify whether the answers being given or the doctors given them on their network is better than just going straight to a nearby specialist. But, he argues, neither can a doctor's visit: HealthTap simply mimics the process of getting a recommended solution in person, exposes it to a broader network, and lets the patient decide from (ideally) a wider buffet of possible choices.
Indeed, it may even incentivize doctors to discuss a point of disagreement more, since they have a vested interest in gaining a network of support. "What HealthTap allows them to do is to go and grow a coalition."
HealthTap does not require board certification, only that they are licensed to practice medicine. In an email expressing concern about HealthTap to the New York Times, American Medical Association President Peter Carmel wrote that he hopes online medical advice can “complement, not replace, the communication between a patient and their physician."
For Dr. Rutledge, HealthTap is about exposing more information than was previously available, which allows users to seek out the best specialist who can help them on and offline. "The user can see who has agreed with the answer, so they can evaluate the evaluator, if you will, through the system," he says. In other words, HealthTap is betting that radical transparency and authentic identities can be as meaningful as the otherwise opaque knowledge network that exists among doctors.
A Translator For Colloquialism
Searching Google for medical answers can often turn up irrelevant or spam-y results. For example, when this question was searched in Google, "Cellulitis from a spider bite, and hepatitis C. Is this serious?," it wasn't easy to find the fact that Hepititus C could be a serious complication. On HealthTap, their new algorithm alerts specialists and returns a potentially more relevant answer: "Hep C which includes interferon are generally immunesupressed. This is serious and need to be started on antibiotics, and may need intravenous antibiotics as soon as possible depending on the severity of infection," wrote one doctor.
In a personal conversation, an experienced physician could quickly translate symptoms and colloquial names into the precise medical language a patient needs to seek more information and the right specialist.
To replicate this in-person experience, HealthTap is launching a comprehensive mapping database, to connect all the conventional search terms to their precise medical code. "For example," writes Gutman, "if someone hears that they’re at risk for Marfan’s disease, do they know that they should see a rheumatologist?"
If their mapping database can better match patients to treatments and doctors than Google, then HealthTap may be on its (ambitious) way to being the default national rating and search destination. Regardless of how successful their system might be, HealthTap has given us a glimpse of how radical transparency and gaming can change the profession of medicine.